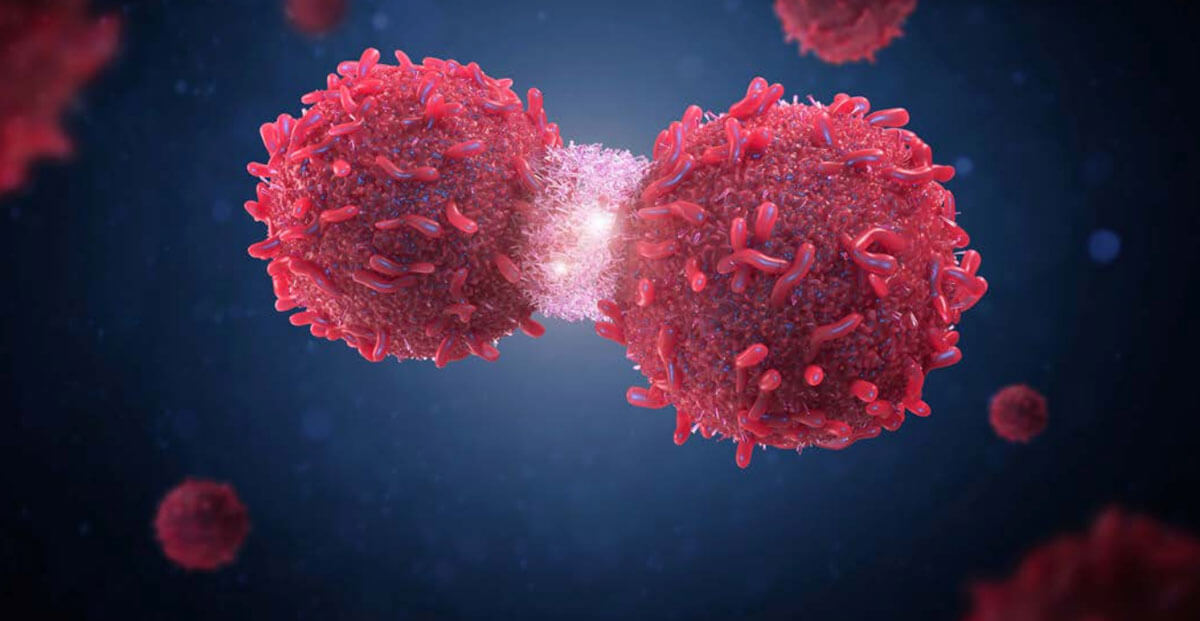
Over the past decade, immuno-oncology (IO) has become one of the most promising and fastest-growing areas of cancer research and drug development. Present-day advances in immuno-oncology can be attributed to an explosion of research in this area in recent years, leading to a paradigm shift in the understanding of cancer.
Until the late 1990s and early 2000s, cancer was considered a disease of genetic origin, with hallmarks including sustained proliferation, resistance to apoptosis, the ability to promote angiogenesis, and the ability to promote invasion and metastasis. This view failed to consider the dynamic nature of interactions between the tumor and its microenvironment – the normal cells in the surrounding tissue as well as the immune system.
Advances in our understanding of the immune system’s dual role in cancer have led to the development of immunotherapies that target both the tumor and its microenvironment. In this white paper, we explore the immune system’s role in cancer development and the history and challenges of developing immunotherapies for cancer.